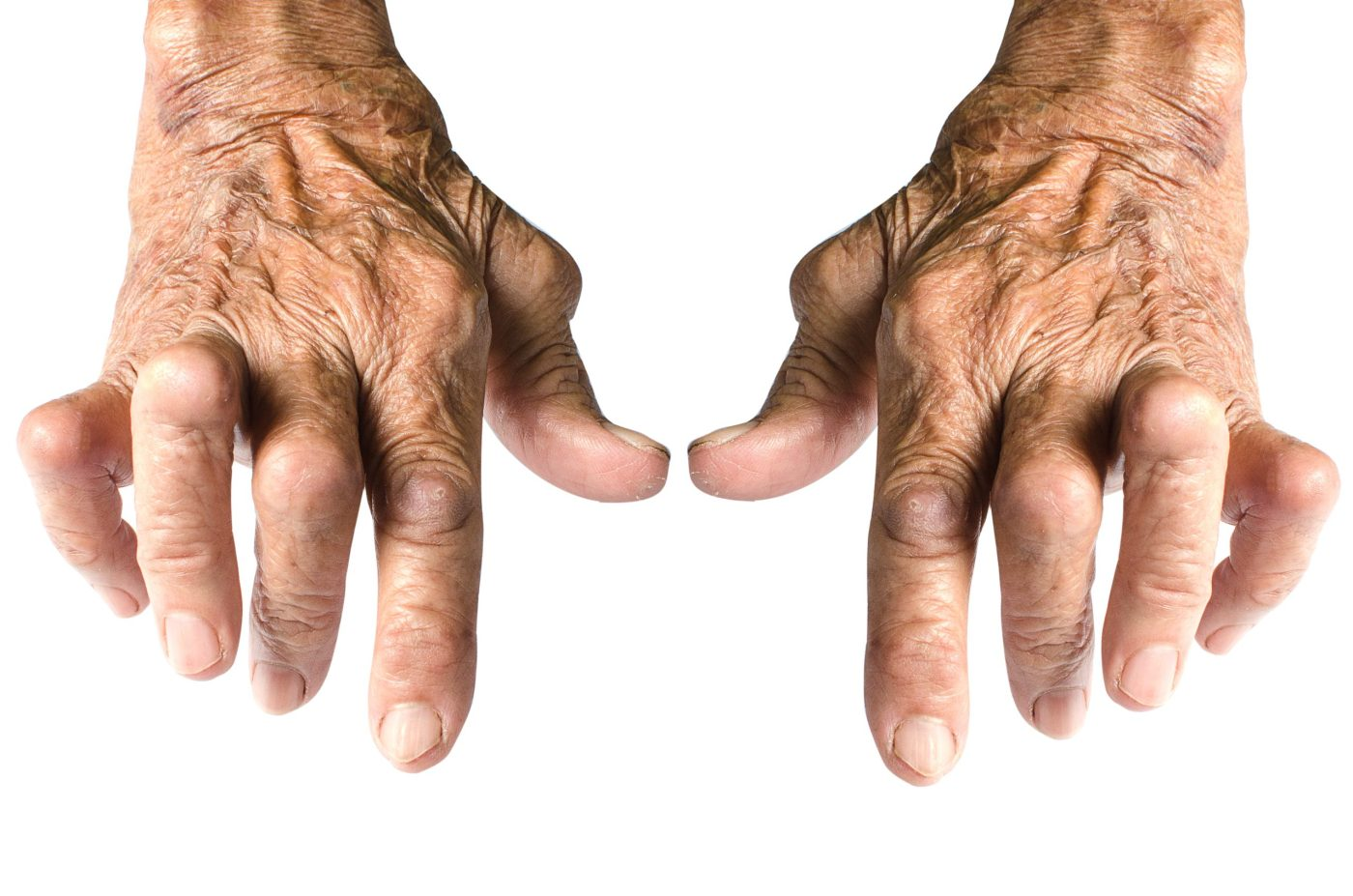
What is Rheumatoid Arthritis?
Rheumatoid arthritis is a chronic autoimmune disease that primarily affects your joints. This means that your immune system (which usually fights infections) attacks the cells that line your joints (synovium) by mistake, causing your joints to be swollen, stiff and painful. Over time, this can damage the cartilage and bone, causing joint deformity and disability.
Rheumatoid arthritis can also affect other tissues throughout the body, causing complications in the eyes, lungs, heart, skin and blood vessels.
What are the symptoms of Rheumatoid Arthritis?
The main symptoms of rheumatoid arthritis include:
- Painful, warm and swollen joints
- Joint stiffness that is usually worse in the mornings and after periods of inactivity
- Fatigue, fever, loss of appetite or weight
Rheumatoid arthritis can affect any joints in the body and usually affects the joints symmetrically (same joints on both sides of the body). The symptoms may vary in severity and may even come and go. In late stages, rheumatoid arthritis can cause joints to deform and partially dislocate.
What are the risk factors of Rheumatoid Arthritis?
The specific cause of rheumatoid arthritis is unknown but several factors have been identified that may increase the risk of rheumatoid arthritis:
- Gender – Women are more likely than men to develop rheumatoid arthritis.
- Age – Rheumatoid arthritis can occur at any age but it most commonly begins in middle age.
- Family history – If a member of your family has rheumatoid arthritis, you may have an increased risk of developing the disease.
- Smoking – Cigarette smoking increases your risk of developing rheumatoid arthritis and can make the disease worse.
- Obesity –Being obese can increase the risk of developing rheumatoid arthritis.
How is Rheumatoid Arthritis diagnosed?
Rheumatoid arthritis is diagnosed by reviewing the patient’s symptoms, conducting a thorough physical examination and doing investigations such as blood tests and imaging studies (X-rays, ultrasounds, MRI). It is best to diagnose rheumatoid arthritis early so that treatment can be initiated early to slow or stop disease progression.
How is Rheumatoid Arthritis treated?
Treatments for rheumatoid arthritis include:
- Short-term medicine to relieve symptoms such as NSAIDs and corticosteroids
- Medicine to slow the disease progression and prevent joint deformity i.e. Disease Modifying Anti-Rheumatic Drugs (DMARDs)
- Second line biologic response agents (Biologics)
- Physiotherapy and occupational therapy
- Surgery
- Lifestyle changes
What are the complications of Rheumatoid Arthritis?
Besides causing joint damage and deformity, rheumatoid arthritis can also increase your risk of developing:
- Dry eyes and mouth – People with rheumatoid arthritis can develop Sjӧgren’s syndrome, a disorder that decreases the moisture in the eyes and mouth.
- Rheumatoid nodules – These are firm lumps under the skin that can be found at pressure points such as the elbows, but can also be found anywhere in the body, such as the heart and lungs.
- Carpal tunnel syndrome – Inflammation of the wrist joints can cause compression of the nerve that serves your hand and fingers, causing you to have numbness of the hand.
- Cardiovascular disease – Rheumatoid arthritis can increase your risk of hardened and blocked arteries, causing heart attacks and strokes. Treatment of rheumatoid arthritis also includes management of cardiovascular risk factors.
- Lung disease – People with rheumatoid arthritis have an increased risk of inflammation and scarring of lung tissues, causing them to have persistent cough and progressive shortness of breath.
- Osteoporosis – Rheumatoid arthritis itself, along with some medicines to treat rheumatoid arthritis, can increase your risk of osteoporosis hence increases the risk of bone fractures.
- Infections – Rheumatoid arthritis itself and medicines to treat rheumatoid arthritis can impair your immune system, leading to increased infections. Hence it is important to protect yourself with vaccinations to prevent infectious diseases.
Can Rheumatoid Arthritis go away?
No, like diabetes mellitus, rheumatoid arthritis is a long-term disease that doesn’t go away. It is a condition that you’ll have for the rest of your life. However, with early diagnosis, prompt treatment and advances in rheumatoid arthritis treatment, more and more rheumatoid arthritis patients are able to have their disease under control and carry out their normal daily activities.